Bilateral axillary aneurysm repair by open surgery: A case report
| Available Online: | September, 2023 |
| Page: | 63-64 |
Author for correspondence:
Laura Isabel Inga Távara
Department of vascular surgery, Santa Lucia University Hospital, Cartagena, Murcia, Spain
Email: lauminem@hotmail.com
doi: 10.59037/hjves.v5i2.50
ISSN: 2732-7175 / 2023 Hellenic Society of Vascular and Endovascular Surgery Published by Rotonda Publications
All rights reserved. https://www.heljves.com
Laura Isabel Inga Távara MD1, Giuseppe Corte MD 1, Jorge Bartolomé Cuenca Manteca MD, FEBVS 2
1 Department of vascular surgery, Santa Lucia University Hospital, Cartagena, Murcia, Spain
2 Head of department of vascular surgery, Santa Lucia University Hospital, Cartagena, Murcia, Spain
Keywords: axillary aneurysm, aneurysm repair, axillary masses, open surgery, axillo-humeral bypass
Abstract
Full Text
References
Images
Abstract
Abstract:
Axillary aneurysms are rare pathologies and although most of them are the result of traumatic events, there is a percentage that is due to atherosclerotic disease or is the result of a degenerative process over time. Once the aneurysm develops, it can cause distal ischemic events and/or neurological symptoms related to embolism or compression. Therefore, the diagnosis and treatment of axillary aneurysms is crucial for the patient. Most of them can be treated effectively by surgical excision and vascular grafting. We present a case of a patient with bilateral axillary aneurysms diagnosed after embolic complications.
Full Text
INTRODUCTION
Axillary artery aneurysms are rare pathologies that usually develop after upper extremity trauma. They may also occur iatrogenically or as a post-stenotic lesion due to thoracic outlet syndrome or due to the chronic use of crutches. Atherosclerosis as a cause of axillary aneurysms is very rare. They usually go unnoticed and asymptomatic, until they produce symptoms of arterial ischemia in the hand and/or neurological symptoms. Fortunately most of them can be treated effectively with surgical excision and vascular grafting.
CASE REPORT
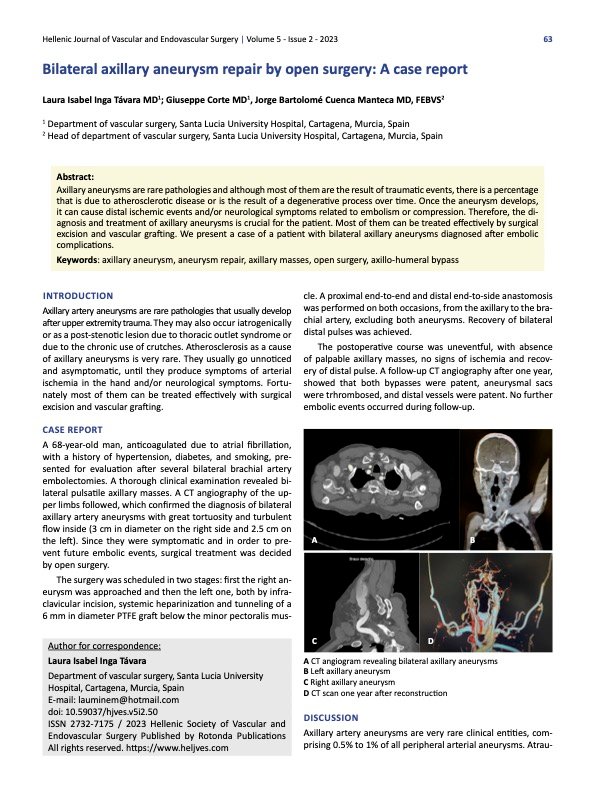
A 68-year-old man, anticoagulated due to atrial fibrillation, with a history of hypertension, diabetes, and smoking, presented for evaluation after several bilateral brachial artery embolectomies. A thorough clinical examination revealed bilateral pulsatile axillary masses. A CT angiography of the upper limbs followed, which confirmed the diagnosis of bilateral axillary artery aneurysms with great tortuosity and turbulent flow inside (3 cm in diameter on the right side and 2.5 cm on the left). Since they were symptomatic and in order to prevent future embolic events, surgical treatment was decided by open surgery.
The surgery was scheduled in two stages: first the right aneurysm was approached and then the left one, both by infraclavicular incision, systemic heparinization and tunneling of a 6 mm in diameter PTFE graft below the minor pectoralis muscle. A proximal end-to-end and distal end-to-side anastomosis was performed on both occasions, from the axillary to the brachial artery, excluding both aneurysms. Recovery of bilateral distal pulses was achieved.
The postoperative course was uneventful, with absence of palpable axillary masses, no signs of ischemia and recovery of distal pulse. A follow-up CT angiography after one year, showed that both bypasses were patent, aneurysmal sacs were trhrombosed, and distal vessels were patent. No further embolic events occurred during follow-up.
DSCUSSION
Axillary artery aneurysms are very rare clinical entities, comprising 0.5% to 1% of all peripheral arterial aneurysms. Atraumatic axillary artery aneurysms secondary to atherosclerosis are rarely seen, and the patients are usually asymptomatic.
The risks of an untreated axillary aneurysm are both vascular and neurological. Vascular complications include aneurysm rupture and thromboembolism, since thrombus within the aneurysm sac is present in 91% of patients. Neurologically, the enlarging aneurysm may cause compression of the brachial plexus, leading to transient or permanent sensorimotor deficits.
In our case, the patient had presented with ischemic symptoms on several occasions, and had been treated surgically by embolectomy. The fact that the patient had an obvious cause of arterial embolism, namely atrial fibrillation, had prevented any further diagnostic investigation for other causes of acute ischemia.
In the literature, axillary artery aneurysms are mostly unilateral. Bilateral axillary artery aneurysms have only been reported in two Marfan syndrome patients. In this case, the physical and laboratory examinations did not reveal collagen tissue disease and the aneurysms were attributed to atherosclerotic disease.
Although literature indicates open surgical resection and repair as the standard treatment, endovascular stenting is being used with increasing frequency over the past few years. Although open repair allows complete resection of the aneurysmal lesion with alleviation of compression on surrounding structures, thus removing the risk of rupture and thromboembolism, the appropriate treatment depends on both patient and surgical factors. Surgical factors that have to be considered i nclude the characteristics of the aneurysm (size, location, anatomical variation) and the availability of endovascular expertise.
Regarding the indication for intervention, most authors recommend operative intervention in symptomatic aneurysms or if the aneurysm measures more than 2 cm in diameter in asymptomatic individuals. For asymptomatic individuals, conservative management may be possible, but complications in up to 50% of patients have been reported, particularly thromboembolism, rupture, and compression on adjacent structures.
In our patient, we decided not to perform endovascular treatment, given the tortuosity of the aneurysms and the probability of endoleak after stent implantation due to the large sizes. Moreover, stent placement near a mobile joint carries the risk of stent deformation or breaking.
Aneurysmectomy and grafting with a saphenous vein is a contemporary treatment of choice for most patients with axillary artery aneurysms because of the favorable long-term patency, but the diameter of the vein may not be enough for bridging large vessels. On the other hand, synthetic grafts have fewer issues with size matching and can be used for medium and large arteries.
In our case, the patient’s history (diabetes, active smoker, and hypertension) increased the risk of future cardiac surgery, in which the saphenous vein would have to be used, and, since he presented bilateral aneurysms, we decided to perform the surgery with a prosthetic conduit.
CONCLUSIONS
To date, surgical graft replacement with resection of the aneurysm is still the standard treatment, although endovascular stenting can be offered as a feasible and successful alternative. Treatment choice should be individuaized, ultimately depending on a multitude of patient and surgical factors. The importance of CT angiography in the differential diagnosis in cases of recurrent acute ischemia of the upper limb should be emphasized.
References
- Hyre CE, Cikrit DF, Lalka SG, Sawchuk AP, Dalsing MC. Aggressive management of vascular injuries of the toracic outlet. J Vasc Surg 1998;27:880-5.
- Malik MK, Kraev Al, Hsu EK, Clement MH, Landis GS. Spontaneuous axillary artery aneurysm: a case report and review of the literature. Vascular 2012;20: 46-8
- Altuwaijri T, Bakhraibah W, Iqbal K, Altoijry A. Axillary artery aneurysm associated with Arteriovenous malforma- tions of the upper extremity: A case report. Int J Surg Case Rep 2021;81:105738.
- Senarslan DA, Yildirim F, Tetik O. Three Cases of Large-Diameter True Brachial and Axillary Artery Aneurysm and a Review of the Literature. Ann Vasc Surg 2019;57:273. e11-273.e15.
- Tham SL, Guo Y, Pang MC, Chng JK. Surgical Management of Axillary Artery Aneurysms with Endovascular Stenting versus Open Repair: A Report of Two Cases and Literature Review. Ann Vasc Surg 2019;58:385.e11-385.e16.
- Tetik O., Yilik L., Besir Y., Can A, Ozbek C, Akcay A, et. al. Surgical treatment of axillary artery aneurysm. Tex Heart Inst J 2005;32:186-8.
- Park SK, Hwang JK, Park SC, Kim SD. Endovascular treatment of a spontaneous aneurysm in the axillary artery. Interact Cardiovasc Thorac Surg 2015;20:140-2.
- Schultz T. Axillary artery aneurysm. Sonography 2014;1:49-51
- Senarslan DA, Yildirim F, Tetik O. Three Cases of Large-Diameter True Brachial and Axillary Artery Aneurysm and a Review of the Literature. Ann Vasc Surg 2019;57:273. e11-273.e15.
- Nekkanti M, Sivagnanam K, Bhat S. Isolated Axillary Artery Aneurysm Causing Peripheral Neuropathy of Upper Limb – A Case Report. J Vasc Med Surg 2015;3:207.


